It’s been quite a long road to get here, but electronic insurance billing is now in beta. What does being in beta mean you ask? Well, it just means that we’ve got some finishing touches to wrap up, but you are free to take it for a test drive. Just like everything else we do, our insurance claims and payment management couldn’t be any easier to navigate. Keeping reading to find out more about our beta and how to become a participant.
What can I do right now during the beta?
The current beta has everything you need to properly get your claims submitted to your payer(s) and receive payment to get your claims closed out. Here’s a quick list of all the things you can do today:
- Integrate and connect to clearinghouse Office Ally for claim submission, scrubbing and processing.
- You can also login to Office Ally if you need to dig deeper into any particular claim file information. We don’t lock you out of your clearinghouse account.
- Setup your list of accepted payers.
- Setup payer specific CPT modifiers.
- Collect and store client insurance information on the client record or let your clients enter their information in the portal.
- Authorization number tracking.
- Copay and deductible tracking.
- Auto-populate and scrub CMS 1500 forms.
- Print formatted and blank CMS 1500 forms.
- Submit electronic CMS forms directly from therapyzen to your payer.
- Get daily claims status updates.
- Modify rejected claims and resubmit electronically.
Feature development in progress during our beta:
The following list of items are currently being finished up with the help of invaluable feedback from our existing users:
- Enter manual EOB or other insurance payment details.
- Mark claims as closed.
- Automatically allocate ERA (Electronic Remittance Advice) payments from your payer(s).
- Submit secondary claims using client secondary insurance policies.
- Client eligibility checks.
- Insurance billing reports.
Why should I participate in a beta?
Great question. Therapyzen has become the super user-friendly tool that it is today by us listening to our users. We’ve been known to take a great suggestion, have it coded and live in production in just a few days. We’re pretty confident that not many of our competitors can say the same. Our insurance billing feature is no exception so we’re giving users the ability to get in early and let us know how to mold this feature into the most user-friendly experience it can be.
Also, by participating and providing invaluable feedback, your claim submission fees will be waived for your first 6 months of usage. Once the beta ends and we are ready to ‘go live’, our fee will be $0.25 cents per claim. You won’t pay a single cent for claim submission (Office Ally fees notwithstanding)
Here’s a sneak peak at some of the highlights of therapyzen’s insurance billing feature…
“One Click’ claim submission that gets you paid faster.
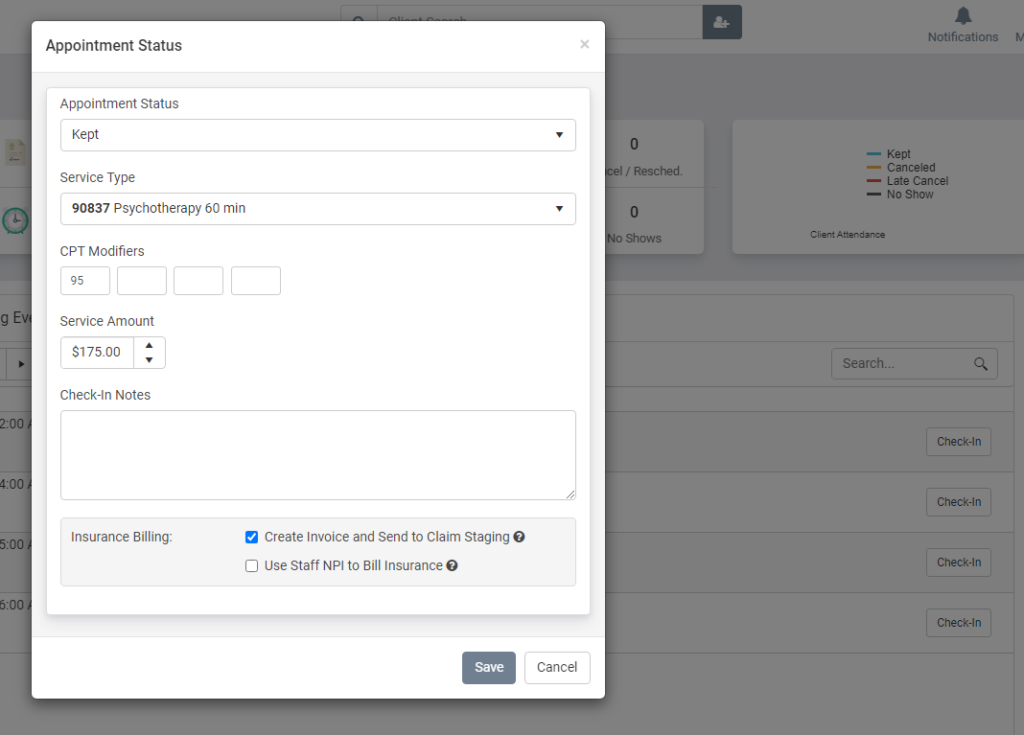
You should not have to jump through a bunch of hoops to get a claim submitted. Not only do we prepopulate all of your CMS files with all of the data needed to get your claim submitted, we let you submit with a single click. For those clients who have all their insurance information populated, just use our existing ‘Check In’ process to mark a client’s appointment as ‘Kept’ and like magic, your file is scrubbed and sent.
Our powerful and informative ‘claims dashboard’.
It’s no secret that we put obsessive effort into therapyzen’s design to create the most user-friendly interfaces. Our claims dashboard is no exception. Manage your CMS files, claim cycles and payments all in one place with ease. You’ll be fed up to the minute information on the current state of everything claims related.

Reduce claim rejections with our ‘double scrub’ working in conjunction with Office Ally.
Making sure your CMS files get thoroughly examined for accuracy before sending them off to your payer is crucial. The fewer rejections for silly mistakes and missing information the sooner you can get paid. Therapyzen will double check your CMS forms for required fields and data integrity prior to sending them to Office Ally. Clearinghouse Office Ally will then do a second integrity check of your claim before sending it over to your payer. This double layer of scrubbing your files can let you rest assured that these files should get accepted by your payers without any hassles.

Ready to learn more or jump right in and participate in our beta?
Whether you are an existing therapyzen user or someone looking for their new favorite new EHR, just send us an email to support@therapyzen.com letting us know you’d like to participate in our beta. We’ll help you get setup and provide any free training you’ll need to get the ball rolling. You can also schedule a free demo here.
Thank you for taking a minute to learn more about this exciting new feature. We look forward to working with you and creating the best user experience humanly possible.
Onward!
The team at therapyzen.

